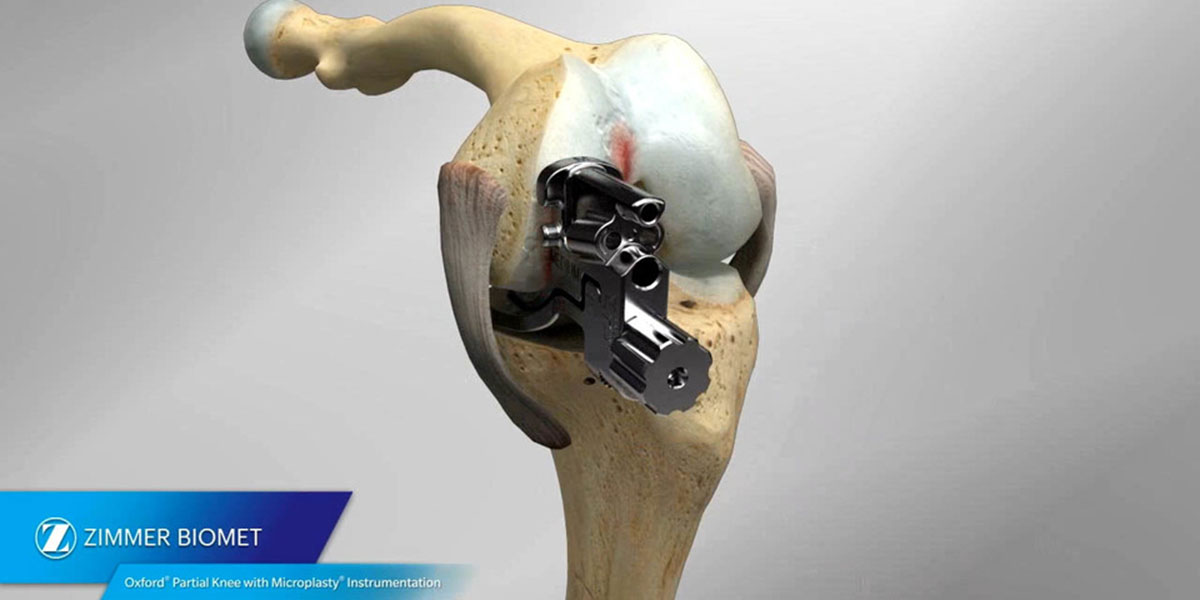
Unicondylar Knee Arthroplasty
Unicondylar Knee Replacement (UKR) or Partial Knee Arthroplasty (TKA), is a type of knee replacement involving only the diseased half of the joint. This is a less invasive procedure that allows for a more natural “feel” after surgery. This is in part, because the cruciate ligaments and half of the knee joint are not touched in the surgery. Overall, the procedure is less invasive than Total Knee Replacement, and the recovery is faster.
Unicondylar Knee Replacement was originally introduced in the 1970’s, and has been modified several time since. Dr. Rodriguez-Elizalde uses the ZimmerBiomet Oxford knee implant, which is the most widely used, and studied partial knee in the world. The current generation of implants and guides make Unicondylar Knee Replacement safe, reproducible and successful.
Partial Knee Arthroplasty is reserved for definitive management of arthritic changes in the knee affecting only one side of the joint. Once the smooth articular surface (cartilage) of the knee is worn out, and pain medication, injections and physical therapy can’t help, surgery may be the answer. It is used primarily to alleviate pain, gain function and restore alignment in the knee.
The key to success in Partial Knee Replacement is ensuring that patients only have arthritis on one side of the knee. In some cases, a “stress” x-ray of the knee will help guide the decision making of Dr. Rodriguez-Elizalde. If there is any involvement in the other half knee, a Total Knee Replacement will be recommended. Sometimes this is only determined at the time of surgery.
Total Knee Arthroplasty involves the surgical replacement of the articular (joint) surfaces of half the knee including the:
1. Bottom part of the Femur (thigh bone), by a cobalt-chromium alloy cap
2. Top part of the Tibia (shin bone), by a titanium metal alloy plate
3. Between the metal pieces, a mobile bearing plastic articular surface is inserted
- FAQ
What is my expected recovery?
You will spend one nights in hospital after your procedure. After you wake up the day of your surgery, you will start to mobilize with a physiotherapist at the side of the bed, and practice transfers to a chair. You can put your full weight on your operated leg, but have to wait until the nerve blocks used for anesthesia wear off, before moving without a knee brace.
Physiotherapy is important in Unicondylar Knee Replacement surgery. The more you move, and push the progression of your range of motion, the better the outcome.
Once safe and comfortable, you will be discharged home with a prescription for painkillers, blood thinners and anti-Inflammatories. You will see Dr. Rodriguez-Elizalde 10-14 days after surgery in the fracture clinic for examine the wound and to check your progress.
The next visit is at 6 weeks, and involves a clinical check and x-rays.
Overall, in terms of recovery, you will likely need a walker or cane for the first 4-6 weeks. A rough estimate of a timeline is a 50% improvement at 6 weeks, and 80% at 12 weeks. The last bit of recovery is mainly endurance training to help combat fatigue and stiffness. This can take up to a year to improve. The most common complaints are stiffness, ache and swelling in the front of the knee. Your deep “arthritic joint” pain should be gone the minute you wake up from surgery, but post-surgical pain in Total Knee Replacement surgery can be significant.
The most important thing to remember is that recovery varies for everyone. Dr. Rodriguez-Elizalde prefers to monitor your progression vs an absolute timeline. As long as you continue to improve week to week, you are doing well.
Back to work?
This question varies a lot on what you do, and any accommodations that can be made for you at work and at home. Most importantly is depends on you – your expectations, drive and recovery are all variable. Most “desk” type jobs can be resumed around 8-12 weeks later, sooner in some cases. Most physical jobs will need a longer recovery, typically 3-4 months.
Driving?
You may drive when:
1) You are no longer taking narcotic pain medication
2) You have full power and function to engage in emergency braking of your car if necessary.
This usually takes a minimum of 6 weeks.
What activities can I do?
After your Unicondylar Knee Replacement has healed, you may return to all day-to day activities. In terms of recreational activities, patients may return to skating, skiing, light weight lifting, swimming, bowling, golfing, tennis, squash, biking and use of an elliptical trainer. The only restriction is high impact jumping and running type activities. This is more Dr. Rodriguez-Elizalde’s personal preference, as there is no direct medical evidence that those activities cause early failure. That being said, running and jumping cause very high joint reactive forces through the knee, and thus are thought to lead to earlier implant failure.
Kneeling can be tolerated in about half of patients post Unicondylar Knee Replacement. The prosthesis is cemented in and can withstand kneeling, but the scar tissue that develops in a lot of patients makes it uncomfortable to knee.
Flying/Travel
Flying and long distance travel should ideally only be done 6 weeks after surgery. Short flights and travel can be undertaken after 7-10 days after surgery, but you should get up and move every hour, and will require a prescribed blood thinner.
The largest hindrance of travel is how you are feeling. You may still need a walker or cane to mobilize safely, and will be moving through crowded areas. Planes, buses and trains are cramped and sitting for long periods of time will cause stiffness and pain in the knee.
In summary, if you are able to delay your travel for the first 6 weeks, you will certainly enjoy your trip more. Short flights, and those necessary for returning home after surgery should not be done before 7 days, and will require a prescribed blood thinner.
Do I need Antibiotics Before a Dental Procedure?
No. This is different than Dr. Rodriguez-Elizalde’s previous recommendations where a dose of antibiotics was given prior to any dental procedure for life.
In reviewing the recent literature and position of the American Dental Association, the use of antibiotics prior to dental work is not necessary. http://www.ada.org/en/member-center/oral-health-topics/antibiotic-prophylaxis
There is no association of hip or knee infection with or without administration of antibiotics before dental work – so we have changed our policy and no longer require you take them.